LASIK
The Blade-Free Advantage
Blade-Free LASIK with the Advanced Precision of IntraLase
Precision and safety are our primary goals in LASIK. To that end, Bloomberg Eye Center brings the latest technology to our patient here in Columbus and Central Ohio. That is why we offer blade-free IntraLase as step one in your all-laser LASIK treatment.
All-Laser LASIK is now approved for Navy pilots and NASA astronauts
With IntraLase, a beam of laser light is used to create the corneal flap, which is then lifted so the second step of LASIK—the reshaping of the cornea—can be done. When the LASIK treatment is over, the flap is securely repositioned into place. This bladeless, computer-guided technology is more accurate than most mechanical microkeratomes (hand-held device with a thin metal blade) that surgeons may also use to create a corneal flap.
IntraLase Assurance and Comfort
IntraLase has been used successfully on hundreds of thousands of eyes in the US, including here in Columbus and Central Ohio, and we trust this advanced technology to deliver exceptional results. Our commitment is to provide you with the ultimate in comfort, safety, and outstanding vision. Blade-free LASIK with IntraLase can help you achieve all of this—while it delivers the added assurance of knowing you’re being treated with the most advanced technology there is.
How IntraLase works
Unlike mechanical instruments, IntraLase technology is uniquely able to program the dimensions of your flap based on what’s best for your eye. Then the IntraLase laser creates your flap from below the surface of the cornea—without ever cutting it. How?
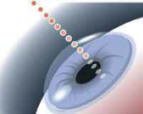
- IntraLase uses ultrafast pulses of laser light to position microscopic bubbles at a precise depth determined by your doctor
- The laser light passes harmlessly through your cornea. Then the laser creating rows of these bubbles just beneath your corneal surface as it moves back and forth across your eye in a uniform plane.
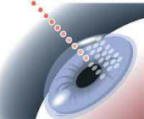
- Next, the IntraLase laser stacks bubbles around your corneal diameter to create the edges of your flap. These bubbles are stacked at an angle that is determined by your doctor and is individualized to the way your eye is shaped.
- The process takes only about 30 seconds from start to finish—it’s quiet and it’s comfortable.
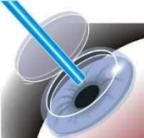
- Your doctor then gently lifts the flap to allow for the second step of your LASIK treatment. When treatment is complete, the flap easily “locks” back into position and rapidly begins to heal.
Blade-Free LASIK is preferred by patients.
The precision of laser-created flaps produces peace of mind for most patients. Blade-free LASIK is truly the safest form of LASIK. In a survey of clinical practices, the vision in the IntraLase-treated eye was preferred up to 3 to 1 by patients over the vision in the mechanical blade-treated eye (among those who stated a preference).
Because of the superior accuracy of IntraLase, certain patients who were ineligible for LASIK may now be able to have treatment. Ask your doctor today if you are a candidate.
The LASIK procedure was simpler than I thought. Now I see 20/20. Bloomberg Eye Center made me feel at ease. I found out how fortunate we are to have Bloomberg Eye Center in our backyard.
